Trudee Hoyte*, Anne Kowlessar, Kevin Henry, Adilah Mahabir, Tichard Manwah and Anil Ali
School of Dentistry, Faculty of Medical Sciences, University of the West Indies, St. Augustine, Trinidad
*Corresponding Author: Trudee Hoyte, School of Dentistry, Faculty of Medical Sciences, University of the West Indies, St. Augustine, Trinidad.
Received: January 18, 2021; Published: February 19, 2021
Ectodermal dysplasia (ED) is a rare heterogenous group of inherited disorders involving ectodermal structures like the skin, nails, hair, teeth and eccrine glands. The most common syndromes are the hypohydrotic ED and hidrotic ED.
This is a case of a 3 year old Afro-Trinidadian female, who presented extra orally with sparse fine scalp hair and eyebrows, soft and dry skin, eczema, a saddle nose, thick everted and protuberant lips. Intra oral findings included hypodontia, dry mucous membranes and conically shaped teeth. The patient was first seen by a paediatric dentist with a presenting complaint of missing teeth and was referred to a dermatologist and an orthodontist.
Keywords: Ectodermal Dysplasia; Hypohydrotic; Hidrotic; Multidisciplinary Approach; Trinidad
Ectodermal dysplasia (ED) is a condition that was first described by Thurmman [1].
It is a rare heterogenous group of inherited disorders that demonstrate developmental defects of two or more tissues and organs which originated from the ectoderm. The defect is in the gene which encodes for protein expressed in hair follicles, eccrine glands and keratinocytes. The tissues affected are the skin, nails, hair, teeth and eccrine glands.
Ectodermal dysplasia disorders are nonprogressive, congenital and diffuse [2,3]. The incidence is around 1 case in 100,000 births with a death rate of 28% in males up to age 3 [4]. The most common syndrome is the hypohydrotic/anhidrotic ED (Christ- Siemens-Touraine syndrome) [5-7], this has an X-linked inheritance pattern; therefore, males are more affected than females. The hidrotic ED (Clouston syndrome) type is inherited in an autosomal dominant pattern [8-10].
Common clinical features include a scarcity of sweat glands and hypohidrosis (inability to perspire and as a consequence, patients experience hyperthermia), onychodysplasia or nail dystrophy, hypotrichosis, partial or total alopecia, dental anomalies and dryness of the mucous membranes [11]. Absence of major salivary glands at birth results in xerostomia, which leads to an increase in dental decay.The general appearance of a person with ED is scanty, blonde fine hair [12]. The eye lashes and eye brows are non-existent or lessened in number. Other features may include sunken cheeks, a depressed nasal bridge resulting in a saddle nose appearance. Around the eyes there is hyperpigmentation, with large low set and pointed ears [13], frontal bossing with thick and everted lips [14].
Intraorally, there can be hypodontia with conical or peg shaped teeth. Anodontia is also likely intraorally and there can be delayed eruption of permanent teeth. Extra orally there may be compromised lip support and a decreased lower face height. Orthopantomography x-rays are an adjunct in diagnosis of ectodermal dysplasia.
An ectodermal dysplasia diagnosis is made when at least two of the atypical ectodermal features occur for example sparse hair and malformed teeth [8,10]. The hair and dentition are affected similarly.
This report is of a 3 year old Afro-Trinidadian female patient who presented with her parents to a paediatric dentist. The patient is an only child and the parents complained that she had multiple missing teeth in the upper and lower arches, spaced dentition and “pointy teeth”.
Extra oral examination revealed that the patient had sparse, very fine scalp hair and eyebrows, soft and dry skin, eczema, a saddle nose, thick everted and protuberant lips (Figure 1 and 2).

Figure 1: Showing patient with fine scalp hair.

Figure 2: Showing fine eyebrows, saddle nose, low set ears and thick everted protuberant lips.
Examination of fingers and toes revealed they were normal shaped with fine brittle finger nails (Figure 3 and 4).
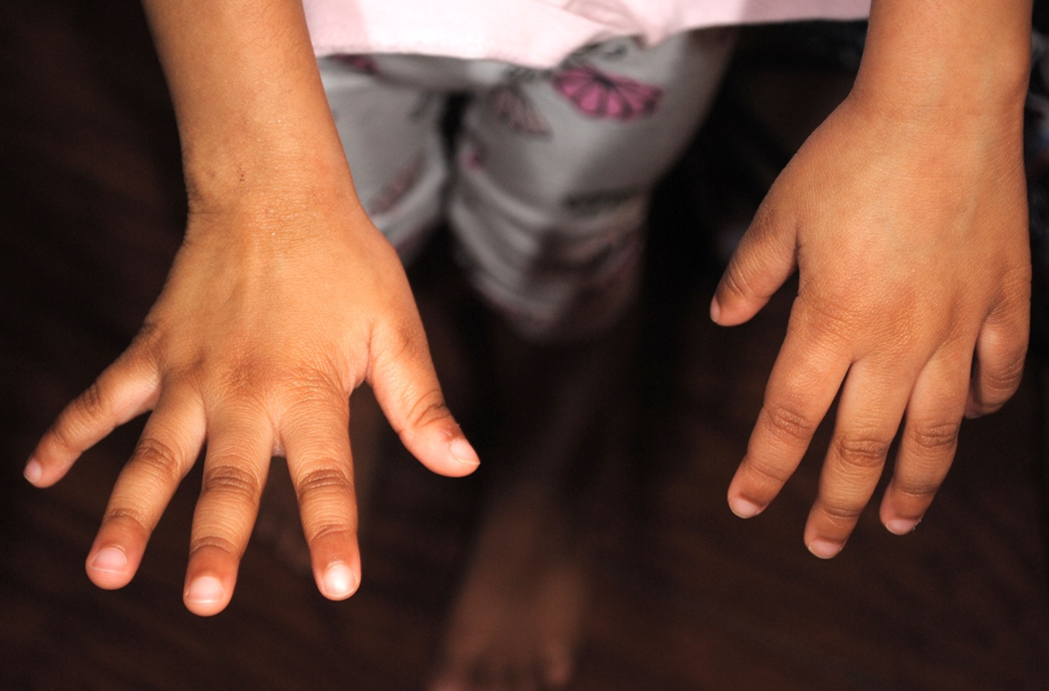
Figure 3: Showing normal shaped fingers with fine brittle nails.

Figure 4: Showing normal shaped toes.
Intra oral examination revealed dry mucous membrane, with three conical shaped teeth in the lower anterior region and nine missing primary teeth (Figure 5).
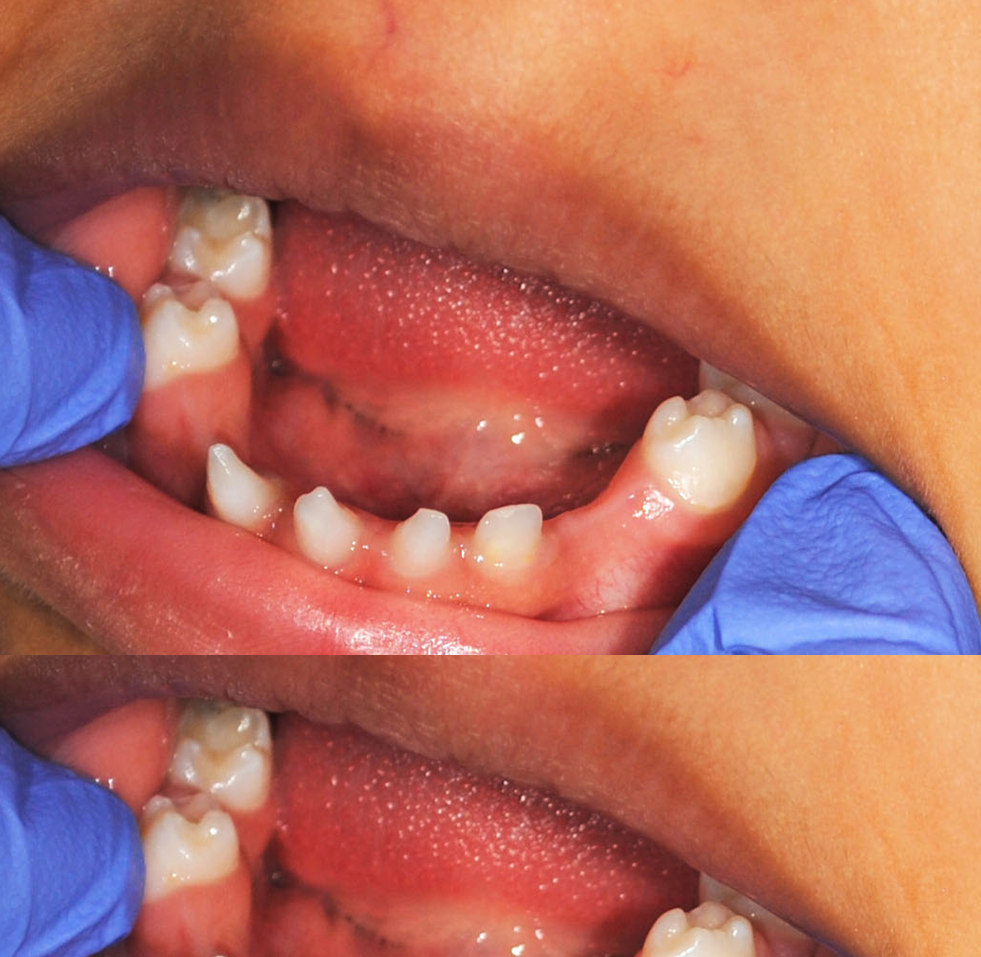
Figure 5: Showing three conical shaped teeth in lower arch
Radiographic examination confirmed multiple absent primary and permanent teeth (Figure 6).

Figure 6: Shows OPG showing conical shaped teeth and hypodontia of primary and permanent dentition.
Parental history revealed no case of ectodermal dysplasia in either family or a history of birth complications during delivery.
Trinidad and Tobago has no reported cases of ED in the literature. This multi-racial society has a sparsity of data on this inherited disorder. It was therefore important to document this case.
TThe earliest classification of ectodermal dysplasia was proposed by Pinheiro and Freire-Maia in 1982 [15]. Here, they used clinical aspects for their classification of ectodermal dysplasia and classified ED into different subgroups based on 1. Eccrine gland dysfunction or dyshidrosis 2. Trichodysplasia or hair anomalies 3. Dental anomalies 4. Onychodysplasia or nail abnormalities.
TThis patient presented with multiple features of ectodermal dysplasia e.g. scanty eyebrows and hair, hypodontia, conically shaped teeth, thin brittle nails, dry mouth and skin.
TThe medical management of ectodermal dysplasia hinges on which ectodermal structure is affected. The patient with dental defects requires early assessment and management. Regular visits should be encouraged with a paediatric dentist to provide preventative and restorative care. Restorative care depending on the severity of the hypodontia can entail removable dentures and in older patients implant retained dentures.
TPatients with reduced lacrimation and xerostomia may benefit from artificial tears and saliva.
TThis patient has her general dental care by a paediatric dentist and she was also referred to a dermatologist and an orthodontist. Parents were also advised to get genetic analysis and counselling to confirm the diagnosis.
THer preventative treatment plan included diet advice (reduce intake of sugary drinks and food), oral hygiene instructions (brush two times daily with a 1500 ppm fluoride toothpaste), fluoride varnish treatments every four months and fissure sealants when permanent teeth erupt. A denture was not indicated since speech and masticatory function were assessed to be adequate. Orthodontic treatment will entail any interceptive orthodontic treatment that is required in the mixed dentition followed by comprehensive multidisciplinary management later on.
TThe dermatologist confirmed the diagnosis of ED and eczema and special creams and washes were recommended.
TThe prognosis for this case is very good with an expected normal life span.
TParents were very concerned about her appearance with multiple missing teeth, this would require a multidisciplinary approach with restorative dentists and an orthodontist as the patient gets older to help improve her self-esteem and quality of life.
A team consisting of medical and dental personnel from different disciplines is required for the multipronged approach to provide comprehensive care to children with ectodermal dysplasia. The paediatric dentist supports dental care, provide prosthesis or devices to support normal function and appearance. Consultation are encouraged with a dermatologist, an otolaryngologist, child psychologist, speech therapist as required.
Citation: Trudee Hoyte., et al. “Ectodermal Dysplasia: Report of a Case in Trinidad". Acta Scientific Dental Sciences 5.3 (2021): 92-96.
Copyright: © 2021 Trudee Hoyte., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
ff
© 2024 Acta Scientific, All rights reserved.